Clinical Department of Oncological Urology

Ladies and Gentlemen, Dear Patients!
In the Clinical Department of Oncological Urology, we are prepared in every respect – training, specialized equipment and organization of medical and nursing care – for the surgical treatment of patients with malignant neoplasms of the genitourinary system: prostate, kidneys, ureters, bladder, penis, testes. The treatment is carried out as part of rapid oncological therapy – a modern organizational solution introduced by the National Health Fund (NFZ), which allows for guiding the patient through the consecutive stages of diagnosis and treatment quickly and efficiently. This system, successfully operating since 2015, may also be known to patients under the terms: Oncological Package, Oncological Card, Oncological Diagnostics and Treatment Card (DILO), “Green Card”.
In order to provide our patients with the fastest possible dates for starting treatment in the Clinical Department of Oncological Urology – we do not admit patients with non-oncological diseases of the urinary system for surgical treatment, e.g. urolithiasis, benign prostatic hyperplasia.
We perform oncological surgeries using classic or minimally invasive techniques (endoscopic / laparoscopic surgeries, percutaneous thermoablative procedures, NanoKnife, etc.). We always make the decision to choose the optimal technique of surgical treatment together with the patient. During the interview, we jointly analyse medical criteria such as: the stage of the neoplastic disease, the patient’s general condition, the risk of complications, quality of life after oncological treatment, and the patient’s preferences regarding the choice of treatment method. In certain situations, it is necessary to plan treatment with different methods in several stages. For this purpose, we arrange a meeting of the patient with a medical committee (case council) composed of doctors of several specialties (urology, radiotherapy, brachytherapy, clinical oncology, radiology). In consultation with the patient, we choose the most advantageous combination of treatment methods from the following: surgery, brachytherapy, radiotherapy, chemotherapy, immunotherapy, hormone therapy, and nutritional treatment.
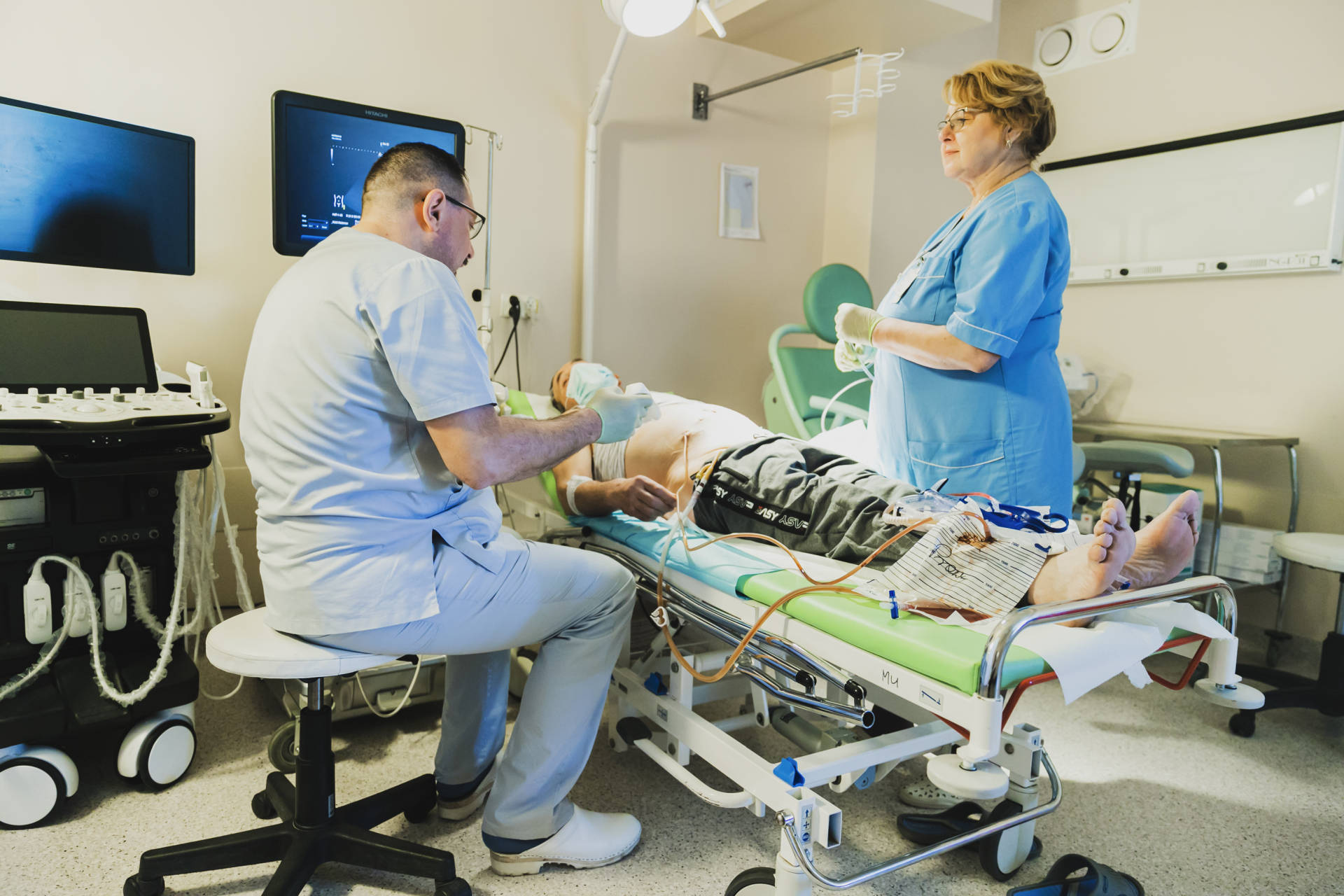
We specialize primarily in the surgical treatment of malignant neoplasms:
- prostate cancer – surgery: radical, classic or laparoscopic prostatectomy – we perform a total of over 250 procedures per year.
- kidney cancer – types of surgery: partial nephrectomy (NSS – nephron-sparing surgery), radical nephrectomy – laparoscopic and classic techniques, in total we perform over 250 procedures per year,
- bladder cancer – types of surgery:
- transurethral resection of bladder tumour (TURBT) – we perform over 500 procedures per year,
- radical cystectomy, radical cystectomy with the formation of a substitute bladder from the small intestine using the Studer method – we perform a total of over 120 procedures per year.
To meet the expectations of our patients, we offer above-standard commercial oncology procedures (payable):
- NanoKnife – a minimally invasive, percutaneous ablation technique that uses electric current with characteristics that cause irreversible damage to cells without causing a thermal effect in them. We perform NanoKnife treatments for properly qualified patients with tumours of prostate, pancreas and liver,
- BiopSee – a technically advanced prostate biopsy performed in the operating room and under general anaesthesia, precisely targeted thanks to the combination of the advantages of two methods of gland imaging: ultrasound and multiparameter magnetic resonance. We perform procedures using the BiopSee technology in cases of high probability of the presence of prostate cancer for patients in whom previous standard biopsies did not confirm the presence of cancer.
- EMDA – intravesical cytostatic therapy (intravesical chemotherapy) using electromotive distribution of the drug to the tissues for properly qualified patients with recurrent bladder cancer.
Patients referred for urological treatment to the Oncology Centre should report with the Diagnostic and Oncological Treatment Card (DiLO) to the Urology Clinic located in the building of THE POLYCLINIC OF THE ONCOLOGY CENTRE. Before arrival, we recommend that you contact the Registration Desk by phone – number: 52 374 31 10 between 7.00 a.m. – 5.00 p.m. on working days. An earlier telephone conversation will allow you to plan the patient’s admission in a timely manner by the appropriate specialist. We strive to ensure that patients arriving for the first-time at the Registration of the Policlinic of the Oncology Centre, with a DILO card – if possible, are admitted to the Urology Clinic by a urologist on the same day. In exceptional situations, with a large number of first-time patients, the date of the visit may be set by the Registration for the following days. There are three admission rooms of the Urology Clinic (Polyclinic, 1st floor: rooms 139, 140, 141) open daily to patients. For an appointment at the Urology Clinic, the patient may come with one accompanying person, who will be authorized by him/her to provide information about the patient’s health. This person is to assist the patient in the course of performing the necessary examinations and consultations, preparing for surgical treatment in the Department of Oncological Urology of the Oncology Centre.
The comprehensive care for patients with oncological disease, organized at the Oncology Centre in Bydgoszcz, is recognized by doctors from other centres and provides the hospital with a permanent place among the best hospitals (nationwide rankings). We care about the comfort of the patient’s stay at the Oncology Centre and we try to reduce the stress related to the awareness of the oncological disease. Patients stay in single or triple rooms with their own bathroom, TV and Internet. If their condition allows it and they do not have to eat by their bed, they go to the restaurant “Fantazja” for meals 3 times a day. Here they stop being patients and become guests of a hotel-standard restaurant, offering a variety of special dishes, soups, desserts and drinks prepared under the supervision of clinical nutritionists. The mental state of patients is taken care of by a team of therapists – clinical psychologists from the Spiritual Support Team. When the SARS-CoV-2 epidemiological situation allows it, cultural life will return to the Oncology Centre. In the afternoons and on days off, when most hospitals stop operating, the Oncology Centre organizes concerts by outstanding artists from the Opera Nova, the Pomeranian Philharmonic Society (Filharmonia Pomorska) and the Academy of Music in Bydgoszcz, who share a passion for art and a desire to create together. The modern Park of Active Rehabilitation and Sport with the Rehabilitation Institute ensures the fastest possible recovery of patients after oncological treatment. Outpatients can use a full spectrum of treatments, gyms, a salt cave, saunas and a full-size swimming pool.
Please have a wheeled bag / suitcase that you do not need to carry. Please take only the essential items:
- ID card;
- a notebook with an organized, complete medical documentation (also CDs with CT and MRI examinations),
- a list of medications taken and medicines in original packaging in the amount needed for 2-3 weeks,
- personal toilet items, a washing sponge, shower flip-flops, slippers, 2-3 sets of pyjamas, towels, a few changes of underwear (men – tight-fitting briefs, not loose shorts are recommended),
- own mug and cutlery – for the comfort of eating,
- please do not take jewellery (rings, earrings), valuables, money, credit cards to the hospital, forego makeup, remove nail polish and tips, do not use contact lenses.
- 1-2 days before admission to the Department of Urology, the date of taking a smear for SARS-CoV-2 infection (coronavirus causing COVID-19) is scheduled. The testing is obligatory for all admitted patients with some exceptions (vaccinated persons, convalescents), which are decided by the doctor at the Urology Clinic who issues a referral to the hospital. The smear collection point is located in front of the Admission Room of the Oncology Centre. After taking the smear, the patient returns home without waiting for the result, which will be available after about 4-5 hours. In the event of a result confirming the infection (the so-called positive result) – a doctor from the department will notify about it by phone and will set a new date of admission to the hospital, postponed by no less than 20 days. No phone call from the doctor on the day of the test means that the result is correct and that the scheduled admission to the hospital is up to date.
On the day of admission to the hospital, you should report to the Admission Room after a light breakfast between 10.00 a.m. – 11.00 a.m., you may be assisted by no more than one accompanying person. From the Admission Room to the Urology Department the patient goes on their own or with the help of designated personnel. In front of the entrance to the Urology Department, on the right side there is the Secretariat Office, where you can confirm your arrival. The secretary will allow you to enter the ward and will indicate the nursing point to approach. At the nursing point, an assigned nurse will ask you some health-related questions, assign you a bed in the hospital ward and tell you how to prepare for the surgery on the following day.
The average length of hospital stay that you need to prepare for depends on the type of surgery planned, for example:
- radical prostatectomy (removal of the prostate gland) – stay from 4 to 8 days.
- nephrectomy (removal of the kidney or its part with the tumour) – stay from 5 to 7 days,
- cystectomy (removal of the bladder) – stay from 9 to 14 days,
- TURBT (transurethral resection of bladder tumour) – stay from 3 to 4 days,
Discharges to home after surgery are carried out daily, also on public holidays, from 11.00 a.m. to 2.00 p.m. Documentation describing the course of treatment is issued by the secretariat office from 11.00 a.m. The excerpt always includes: medical recommendations, nursing recommendations, dietary recommendations, prescriptions, on request – a certificate of incapacity for work. Recommendations are the most important part of the discharge documentation – they contain information on the date of a follow-up appointment at the urology clinic, care of the surgical wound, and dosage of prescription drugs.

|
Department Coordinator
Krzysztof Kamecki, MD, PhD
|
|
Head of Medical Care
Katarzyna Kisiel, MSc
|
On the day of admission to the Urology Department, the doctor conducts an interview with the patient, checks the preparation for the operation and receives a signature on the informed consent form. Consent forms for the most frequently performed operations are available below:
- consent for radical removal of the prostate gland – classic technique,
- consent for radical removal of the prostate gland – laparoscopic surgery,
- consent for radical kidney removal surgery – classic technique,
- consent for radical kidney removal surgery – laparoscopic procedure,
- consent to surgery to remove part of the kidney with the tumor – classic technique,
- consent for surgery to remove part of the kidney with the tumor – laparoscopic procedure,
- consent to the operation to remove the bladder and to divert the urine to a urostomy – classic technique,
- consent to the operation to remove the bladder and to divert the urine for urostomy – laparoscopic procedure,
- consent to the surgery to remove the bladder and create an intestinal reservoir for urine (Studer method) – classic technique,
- consent to the procedure – removal of the bladder tumor through the urethra – endoscopic procedure.
Odwiedziny
- odbywają się codziennie w godzinach od 15.00-17.30,
- rekomenduje się wejście na oddział tylko 1 osoby odwiedzającej,
- osoby z objawami infekcji nie mogą odwiedzać pacjentów,
- przypominamy o obowiązku noszenia maseczki podczas całego pobytu w Centrum Onkologii
Przyjęcie do Oddziału
Izba Przyjęć znajduje się na niskim parterze w tylnej części Budynku Głównego. Z jej usług korzystają osoby skierowane do planowanej hospitalizacji oraz pacjenci leczeni w Centrum Onkologii, u których nastąpiło nagłe pogorszenie stanu zdrowia.
Pacjenci zgłaszający się do przyjęcia powinni mieć dowód osobisty lub inny dokument potwierdzający tożsamość.
Po rejestracji w Recepcji Izby Przyjęć chory udaje się do przebieralni, jeśli zachodzi taka potrzeba pielęgniarka/ sanitariusz pomaga choremu przy przebraniu się. Pacjent przekazuje okrycia wierzchnie rodzinie lub pozostawia je na przechowanie w depozycie szpitalnym. Na oddział docelowy chory udaje się sam lub jeśli zachodzi taka potrzeba jest zaprowadzony lub przewieziony przez sanitariusza Izby Przyjęć.
UWAGA!
Szpital nie ponosi odpowiedzialności za rzeczy pozostawione w szafkach przy łóżku chorego, dlatego też wszelkie wartościowe przedmioty (np. pieniądze, biżuteria, karty płatnicze) należy zostawić w domu lub przekazać do Depozytu Rzeczy Wartościsiowych mieszczącego się w Kasie Centrum Onkologii.
Co zabrać ze sobą do szpitala?
- leki oryginalnych opakowaniach + dokumentację medyczną + nagrania płyt z badaniami
- piżamę,
- ręcznik,
- kapcie, klapki pod prysznic,
- wygodne ubranie bawełniane np. dres,
- bieliznę osobistą,
- szlafrok,
- środki czystości (mydło, szampon, szczotkę i pastę do zębów, dezodorant)
- przybory toaletowe (grzebień, przybory do golenia itd.)
Co można zabrać:
- sztućce,
- kubek,
- wodę mineralną niegazową,
- kawę/herbatę,
- chusteczki higieniczne,
- środki higieny osobistej (podpaski),
- książki, czasopisma,
- telefon komórkowy + ładowarkę

